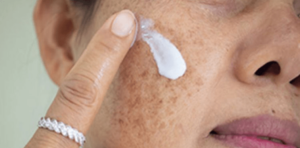
SITE OF OCCURRENCE
Melasma appears most commonly on your cheeks, nose, chin, above the upper lip and the forehead. It sometimes affects your arms, neck and back. In fact, melasma can affect any part of your skin that is exposed to sunlight. That’s why most people with melasma notice that their symptoms worsen during the summer months.
Melasma is a very common skin disorder, especially among pregnant women. 15% to 50% of pregnant women get it. Between 1.5% and 33% of the population may get melasma and it happens more often during a woman’s reproductive years and rarely happens during puberty. It usually starts between 20 and 40 years of age.
Your epidermis contains cells called melanocytes that store and produce a dark color (pigment) known as melanin. In response to light, heat, or ultraviolet radiation or by hormonal stimulation, the melanocytes produce more melanin, and that’s why your skin darkens.
There are three types of melasma and they have to do with the depth of the pigment. A Wood lamp that emits black light may be used to determine the depth of the pigment. The three types are:
- Epidermal: Epidermal melasma has a dark brown color, and a well-defined border, appears obvious under black light and sometimes responds well to treatment.
- Dermal: Dermal melasma has a light brown or bluish colour, a blurry border, appears no differently under black light and doesn’t respond well to treatment.
- Mixed melasma: Mixed melasma, which is the most common of the three, has both bluish and brown patches, shows a mixed pattern under black light and shows some response to treatment.
Melasma is harmless. It’s not painful, itchy, or uncomfortable in any way. Melasma is a typically chronic disorder. This means that it’s long-lasting (three months or more). Some people have melasma for years or their entire lives. Other people may have melasma for just a short time, such as during pregnancy.
- Antiepileptic medications
- Contraceptive therapy (birth control)
- Genetics
- LED Screens
- Pregnancy
- Hormones
- Makeup (cosmetic item)
- Phototoxic drugs (medicines that make you sensitive to sunlight)
- Skin care products
- Soaps
- Tanning beds
Melasma can sometimes be mistaken for another skin condition. To tell the difference between skin conditions, your healthcare provider may perform a biopsy, which is where a small piece of your skin is removed and examined. A biopsy is quick, safe procedure routinely performed during a normal visit to your healthcare provider’s office. Skin conditions commonly confused with melasma include:
- Actinic lichen planus and lichen planus.
- Drug-induced pigmentation.
- Guttate hypomelanosis.
- Hydroquinone-induced exogenous ochronosis.
- Lentigo (age spots).
- Nevus of Hori.
- Nevus of Ota.
- Postinflammatory pigmentation.
The severity of your melasma can be measured by using the Melasma Area and Severity Index (MASI). Your healthcare provider may administer the test.
If you have melasma, be sure to avoid:
- Hormone treatments, specifically ones that involve estrogen.
- Birth control, specifically oral contraceptive pills contains estrogen and progesterone.
- LED light from your television, laptop, cell phone and tablet.
- Makeup you find irritating to your skin.
- Medications that may cause or worsen melasma.
- Scented soaps.
- Skin care products that irritate your skin.
- Tanning beds.
- Waxing, which can aggravate the melasma.
Is melasma curable?
Melasma may fade on its own in some women. This is most common when it is caused by pregnancy or birth control medications. There are lotions that your doctor might recommend to brighten your skin. Topical steroids may also be used to help lighten the afflicted regions. Chemical peels, dermabrasion, and microdermabrasion are further alternatives if they do not work. These procedures remove the top layers of skin, which may help lighten dark spots.
These methods do not ensure that melasma will not return, and certain cases of melasma cannot be entirely removed. To decrease the chance of the melasma returning, you may need to return for follow-up appointments and adhere to specific skin care habits. These include limiting your sun exposure and using sunscreen on a daily basis.
Treatment
Cell restore therapy for Melasma
Stem cells are master cells in the human body that can divide and generate duplicates of themselves as well as many other types of cells. They can be found in many different areas of the human body at every stage of development, from embryo to adult. The stem cells utilised in this study are mesenchymal stem cells obtained from bone marrow. These are multifunctional stem cells that can differentiate into a number of cell types to aid in the regeneration and repair of damaged tissues.
Skin diseases are classified as autoimmune diseases since the body's own immune system attacks and damage the skin's colour-generating cells. Immunosuppressive and immunomodulatory characteristics of mesenchymal stem cells have been discovered. In vitiligo, administering mesenchymal stem cells will prevent additional damage to melanocytes and slow the course of the illness. If an unstable vitiligo can be stabilised, additional procedures like as surgery can aid with ongoing care. Over time, the mesenchymal stem cells will increase pigmentation. The objective of stem cell treatment in vitiligo is to repair the skin's damaged colour-generating cells while also correcting the faulty immune system.
Because stem cells are so adaptable, they might be utilised to repair and replace damaged human tissue. The goal of experimental stem cell treatment for skin conditions is to give possible benefits of stem cells that will reduce or stop future deterioration caused by the illness and to determine whether the stem cells can cure the disease's symptoms. For the best dermatologist in Gurgaon Contact Lamidas Skin Care.